

Medical Lifestyle Assessment
How Much Does Lifestyle Dictate Health?
Comprehensive Diagnostic Evaluations at J. Flowers Health Institute
The information presented on this page is an overview of the average evaluation of this nature and is offered here as a resource. At J. Flowers Health Institute, our evaluations are customized and tailored to the individual’s needs. We specialize in providing truly comprehensive health and wellness evaluations and a workable plan for future health to those who want to improve their quality of life.
If you would like to learn more about J. Flowers Health Institute, please do not hesitate to reach out.
How Does Lifestyle Impact Health?
Table of Contents
Why is a lifestyle assessment important for your medical care? In current society, it is more popular to take medication than to make lifestyle changes, even when those changes could improve overall health. The reality is that many diseases and disorders today are preventable and can be managed with the right lifestyle choices. Lifestyle assessments give your medical professional detailed information to help properly decide what care you need.
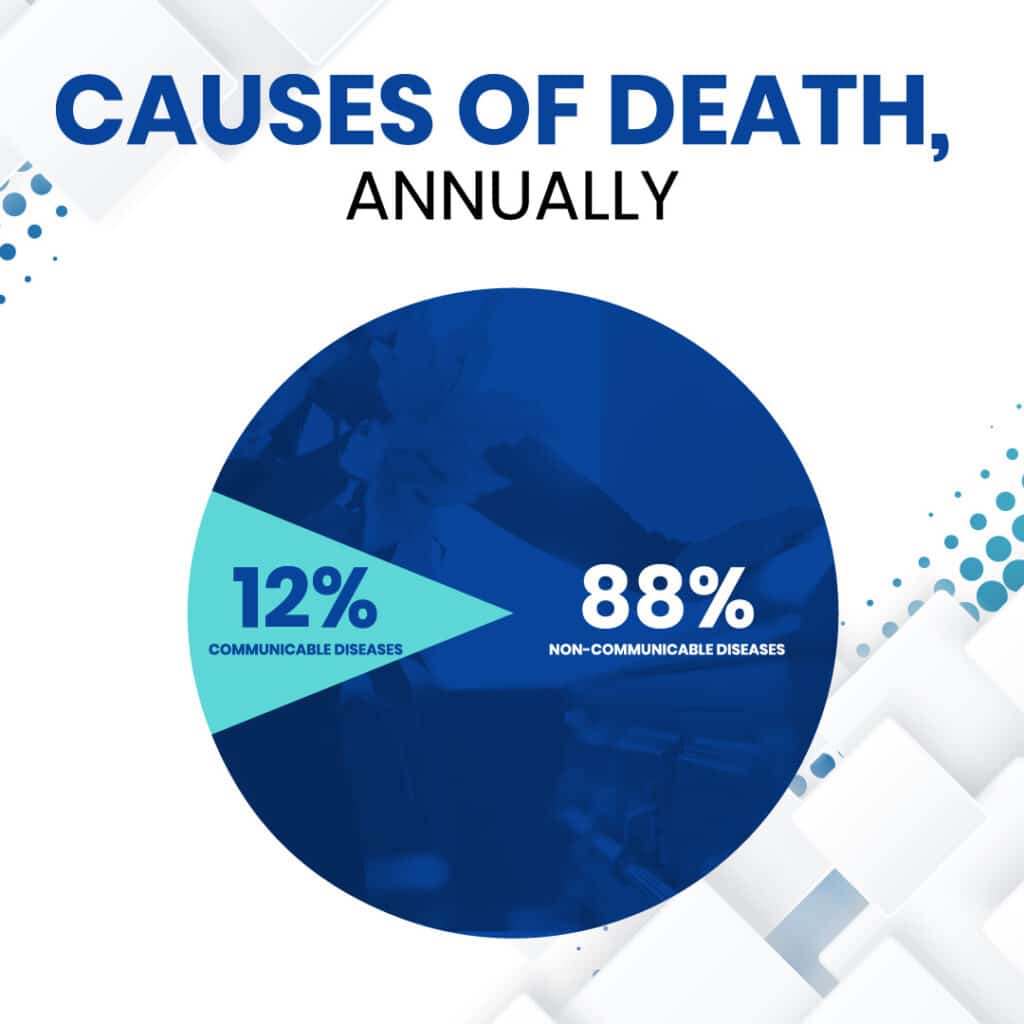
Non-Communicable Disorders
- Cardiovascular diseases
- Cancer
- Chronic respiratory diseases
- Diabetes
- Obesity
- Hypertension
- Stress
- Anxiety
Cardiovascular Diseases
Cardiovascular diseases (CVDs), specifically coronary heart disease and strokes, are the leading cause of death globally and in the United States. CVDs can be largely prevented by addressing the following risk factors and lifestyle habits: tobacco use, unhealthy diet, obesity, physical inactivity, and diabetes.
Cancer
Chronic Respiratory Diseases
Diabetes
Share This Article
Categories
Top Blogs
Recent Post
Lifestyle Habits
Most of the modern-day healthcare system is reactive, meaning that people typically go to the doctor once they have a problem that they need to address. Preventative healthcare focuses more on adopting healthy lifestyle habits in order to prevent and avoid certain diseases that cause premature death.
What is a Medical Lifestyle Assessment?
A medical lifestyle assessment involves the collection and analysis of health-related information that is then used by clinicians and healthcare teams to support healthy behaviors and change harmful behaviors. This process is completed with a healthcare provider where a patient provides an overview of lifestyle habits, such as dietary habits, physical exercise, drinking or smoking habits, drug use, sleep patterns, stress levels, and more. This assessment gives primary care teams the opportunity to examine a patient’s health status for potential health risks in order to help prevent NCDs.
What Health Concerns are Typically Discussed in a Lifestyle Assessment?
- Dietary habits
- Physical activity
- Depression
- Anxiety
- Social support/social isolation
- Alcohol/substance abuse
- Sexual activity
- Tobacco use
- Personal safety
- Pain
- Ability to manage your own health
- Quality of life
- Any other health behaviors, risks, or concerns
Who Performs a Lifestyle Assessment?
In a typical lifestyle assessment, a lifestyle assessment form will be completed that involves a list of questions, which will then be discussed with a doctor. Any changes to health or healthcare plans that are implemented as a result of a lifestyle assessment may involve other health care providers, such as specialists, psychologists or psychiatrists, nutritionists, personal trainers, social workers, and more. After completing a lifestyle assessment, the patient and their healthcare provider will make a plan of action in order to address any problems or concerns.
What are the Benefits of Medical Lifestyle Assessments?
- Improving the patient-healthcare provider relationship by creating rapport and having a dialogue surrounding current health.
- Giving patients the opportunity to talk about issues that might be sensitive to some people, such as mental health issues, alcohol or drug use, and sexual activity.
- Helping healthcare providers identify and prioritize patient health issues and goals.
- Providing patients with information and education surrounding how lifestyle habits can impact health.
- Helping patients understand their health status and step to improve their health.
- Reminding patients to be aware of behaviors and habits that affect health or are risk factors for chronic conditions.
- Tracking patient health behavior over time and improving patient follow-up.
- Measuring and monitoring patient data at the population level for proactive care.
- Identifying issues that might require referrals, specialist help, or additional resources.
How is a Lifestyle Assessment Performed?
General Information
- Name
- Date of birth
- Marital status
- Number of children
- What are your main health concerns?
- How are you feeling?
What are you doing for your health presently?
- Exercise
- Healthy diet
- Chiropractor
- Medical doctor
- Vitamins
- Minerals
- Herbs
- Prescription medications
- Relaxation techniques
- Acupuncture
- Meditation
- Other
- What do you believe might be the causes or underlying factors of your current health concerns?
Life Stress
- Have you experienced any trauma or loss in the past?
What level of stress are you experiencing during this time of your life?
- Minimal
- Average
- Considerable
- Unbearable
- What does your stress look like?
- Do you have any coping mechanisms for your stress?
What are the major causes of stress in your life?
- Financial
- Career
- Personal
- Marriage
- Relationships
- Mental Health
- Physical Health
- Family
- Spiritual
- Unfulfilled expectations
- Other
Sleep Habits
- How many hours do you sleep daily on average?
- What time do you go to sleep?
- What time do you wake up?
What time do you wake up? Do you wake up feeling rested?
- Financial
- Yes
- No
- Sometimes
- What is your typical energy level?
Daily Life & Exercise
- What is your occupation?
- How many hours do you work every day?
- What time do you start and end work?
Do you enjoy your work?
- Yes
- No
- Sometimes
Do you smoke cigarettes?
- If yes, how many?
- If no, are you ever exposed to second-hand smoke?
How many hours do you spend daily, on average:
- Driving
- Watching TV
- Reading
- On social media
- Using your computer
- Walking
- What do you do for exercise?
- How frequently do you exercise?
- What are your interests and hobbies?
- Do you take vacations regularly?
- When was your last vacation?
- Do you actively participate in a church or spiritual group?
Medical History
- Height
- Weight
- Do you wish to gain or lose weight?
- Do you have high blood pressure or low blood pressure?
- How much weight would you like to gain or lose?
Are you currently taking any medications?
- If yes, list the medications and reasons for taking them
- List any vitamins, minerals, herbal, and homeopathic remedies you are currently taking and the amounts/dosages you are taking
- Do you have any allergies or sensitivities?
- How often do you have a bowel movement?
Have you ever been hospitalized?
- If yes, for what reason?
Have you ever been diagnosed with an illness, mental or physical?
- If yes, explain what and when you were diagnosed
Do you have trouble having a bowel movement?
- If yes, is it related to a particular food or circumstance?
Do you have loose bowel movements?
- If yes, is it related to a particular food or circumstance?
Have you ever been treated for alcohol or substance abuse?
Females
- Are you or could you be pregnant?
- Are you pre-menopausal or post-menopausal?
Are you experiencing menopausal symptoms?
- If yes, specify what symptoms
Have you had a bone density test?
- If yes, what were the results?
Family History
Has your father, mother, sibling, grandparent, sibling, or another relative ever had:
- Heart disease
- Hypertension
- Cancer
- Diabetes
- Arthritis
- Osteoporosis
- Allergies
- Mental illness
- Intestinal disease
- Other
Dietary Habits
How many times a day do you eat?
- How many main meals do you eat? What times of the day?
- How many snacks do you eat? What times of the day?
Do you eat meals:
- With family
- Alone
- At home
- In a restaurant
- On the run
- Fast-food
How many times a day do you eat?
- How many main meals do you eat? What times of the day?
- How many snacks do you eat? What times of the day?
Do you feel like there are restrictions on your diet due to the preference of others? (Family, roommates)
- If yes, explain
Do you feel like there are restrictions on your diet due to the preference of others? (Family, roommates)
- Breakfast
- Lunch
- Dinner
- Snacks
At what time do you have your last meal or snack of the day?
How many ½ cup servings of each do you typically eat in a day?
- Fruit
- Vegetables
- Whole Grains
- Protein
- Dairy Products
Things You Use
Do you eat or use:
- aluminum pans
- microwave
- margarine
- candy
- fried foods
- cigarettes
- artificial sweetener
- fast foods
- air fresheners
- scented body products
Things You Use
Do you eat or use:
- aluminum pans
- microwave
- margarine
- candy
- fried foods
- cigarettes
- artificial sweetener
- fast foods
- air fresheners
- scented body products
Things You Drink
Please indicate how many cups of the following you drink per day:
- Water
- Coffee
- Tea
- Fruit juice
- Vegetable juice
- Milk
- Soft drinks
- Beer
- Wine
- Liquor
- Other
Are you
- A meat-eater
- Vegan
- Vegetarian
- Pescatarian
- Other
- How often do you eat meat?
- How often do you consume dairy products?
- What are your favorite foods?
- How often do you eat them?
- What foods do you crave?
- Do you experience any symptoms if you miss a meal?
- Do you experience any symptoms after eating?
- Is there anything else health or lifestyle-related that you would like to share?
Are there any foods that you avoid?
- If yes, why?
What Information Does a Lifestyle Assessment Give?
Essentially, a lifestyle assessment helps a person be informed and proactive with their health. It teaches how lifestyle choices impact health outcomes. It also helps doctors be more informed about their patient’s health and gives them the opportunity to create an action plan.
How Do Lifestyle Assessments Help Doctors?
Better Understanding
Public Health
This helps healthcare professionals to learn about the effects and outcomes of different medications patients take or health interventions that have been implemented. It helps healthcare professionals to understand how certain lifestyles might relate to specific populations, age groups, genders, and more, and how much lifestyles have effects on health outcomes. Providers are then able to compare and contrast different lifestyles and measure how these affect health outcomes.
How Do Medical Lifestyle Assessments Help the Public?
Resources
- https://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases
- https://www.kff.org/global-health-policy/fact-sheet/the-u-s-government-and-global-non-communicable-diseases/
- https://www.who.int/nmh/countries/usa_en.pdf?ua=1
- http://www.theraheals.ca/wp-content/uploads/2018/03/LAF_E-Form-Feb2017.pdf





